 Medical cover has become expensive. These days, even a minor operation can have you digging into your long-term savings. The high cost of hospital stays, specialist fees and other medical expenses makes it important to have at least some form of medical cover. With all this need for cover a friend or family member might mention to you, different medical aid options or that you must consider medical insurance. This may then get you to ask yourself, what is the difference between Medical Aid and Medical Insurance? Below we provide all the information you’ll need to make the right choice for you and your family. Regulation In South Africa, all medical aid schemes are regulated by the Medical Schemes Act and governed by the Council for Medical Schemes. Health insurance, on the other hand, is regulated by the long-term insurance act and governed by the Financial Services Board. Price One of the most noticeable differences between the two types of cover is the price. Medical aid schemes are notably more expensive, with higher monthly contributions. Medical insurance, however, is far more affordable, but this means there are limitations when it comes to what is covered. You should always consider your health needs when deciding which is best for you. Benefits Medical aids provide Prescribed Minimum Benefits (PMBs) for a list of chronic disorders. Medical insurance plans usually focus on daily health care, such as doctors’ visits and short-term medication. A more comprehensive health insurance plan may offer hospital care in the event of an accident or emergency, to a fixed sum. Although a medical aid plan provides more comprehensive cover, it doesn’t generally include personal accident disability or cover for loss of limbs. Health insurance does. It may also include death and funeral cover, which medical aid schemes do not offer. Medical aid schemes offer comprehensive hospital cover, usually for a large variety of in-hospital treatments, depending on your plan. However, there is often a shortfall between medical aid rates and the rates charged by the medical practitioners. (Therefore, Gap cover is always recommended, so to cover for any shortfalls that may occur) Medical insurance does not cover extensive hospital benefits. Hospitalisation is usually limited to accidents and emergencies and only covers specified costs. If costs exceed the limits, members will have to pay for the extra. Medical aids are also required to cover chronic medication, while medical insurance is not. Tax benefits Medical aid contributions are deductible for tax purposes whereas health insurance premiums are not. To apply for cover, contact our healthcare consultant Tammy email: service@daberistic.com tel:(011)658-1333
0 Comments
“Our Pandemic Shield policy is the first of its kind on the African continent, providing an affordable solution that pays out a lump sum stated benefit if the policyholder is hospitalised as a result of being positively diagnosed with COVID-19 – or any other World Health Organisation declared pandemic illness in the future. The benefit trigger is a hospital admission longer than 48 hours,” adds Martin. Who is Pandemic shield for? Anyone can apply. There are no medicals, and no person will be excluded. Why emplyees need Pandemic Shield Cover? Employees get a lump sum benefit and daily cash amounts if they are hospitalised because of any disease or health event declared as pandemic by World Health Organisation (WHO) What about COVID-19? Any hopitalisation longer than 48 hours, as a result of COVID-19, or SARS-CoV-2 is covered as long as you have been tested positive. Vaccinate your employees' financial wellbeing against COVID-19
*No initial waiting period will be applied but subseqient claims will be subjected to a 21 day waiting period after discharge. *Compulsory groups on Gold and Diamond larger than 50 employees will receive a discount. *Premium and benefits are not gauranteed for the duration of cover and may be reviewed from time to time based on risk factors. *This is not a medical scheme and the cover is not the same as that of a medical scheme. *This policy is not a substitute for medical scheme membership. To speak to a Medical Aid Consultant, please email service@daberistic.com,
Tel 011-6581333, Option 2 for Medical Aid.
3. Good nutrition isn't all about what you don't eat, it's often just as important to add in more nourishing nutrients. This ensures you get enough vitamins and minerals.
Try slicing up raw veggies and keeping them bagged in the fridge as snacks, far easier to grab when they're already bite sized. 4. Another simple, festive trick to up your fruit and Veggie intake. Eat as much of the rainbow as you can. At each meal, see if you can introduce one more colour to your main or side dish. 5. Some call them nature's candy - for good reason. Fruits make excellent desserts, and they are also a key part of a healthy diet, filled with disease-fighting nutrients. 6. Skipping breakfast will likely make you hungrier later in the day, and more prone to overeating unhealthy foods. Morning meal represents a prime opportunity to boost your diet with produce. 7. A good night's rest can also go a long way in keeping you on track. When you are sleep deprived, you are more likely to eat mindlessly and crave high-fat, high-sugar foods. 8. Walking is a good way to fit more activity into your day. Breathing fresh air and seeing different scenery is good for metal health and depression. Getting your blood circulating will assist in reducing your risk for chronic health conditions. Please be reminded that Medical aid upgrades for 2021 will end soon, please make sure you have submitted your change by 30 November. For clients on Discovery KeyCare plan, Momentum Ingwe plan, Bonitas Boncap plan and have been selected to do income verification, please make sure all required documents are submitted to prevent your service provider resulting to default to the highest income band and therefore the highest contribution will apply.
Please note: Members joining Momentum health Ingwe option with effect 01 October 2020 onwards will not be required to submit information for income verification (declaration and proof of income). They will remain on their current income bracket moving into 2021 and the new premium will automatically be applicable from 01 January 2021. For more information on medical aid plans, please see below videos, brochures and links to assist you with change of option decision. Discovery Plan series and videos
Below are Discovery Health Plan Guides Brochures for 2021
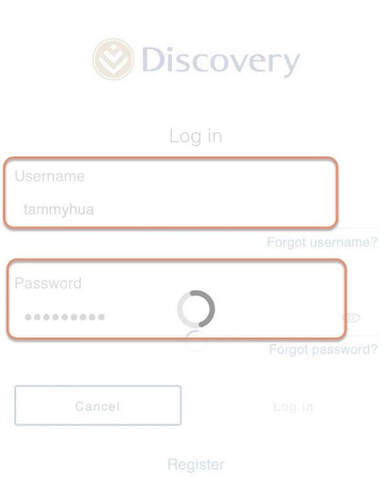
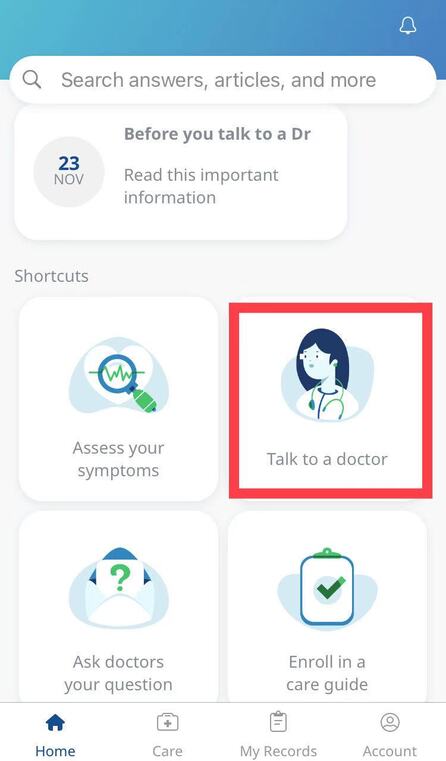
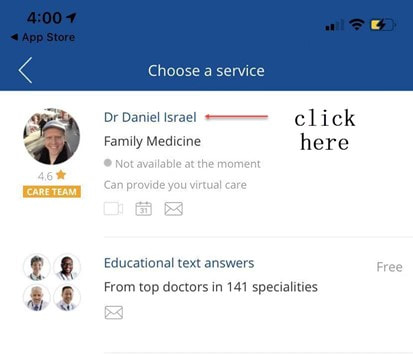
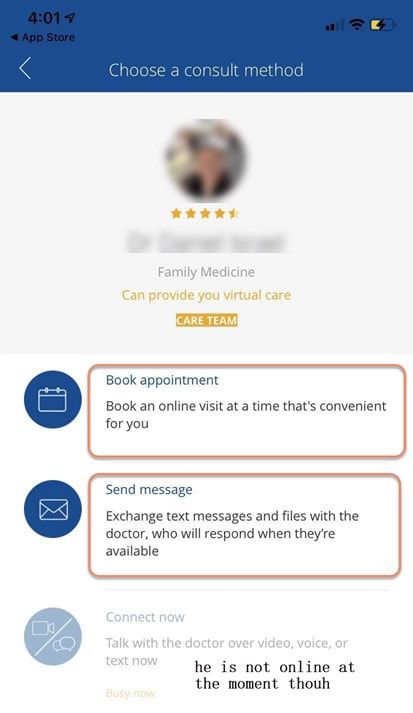
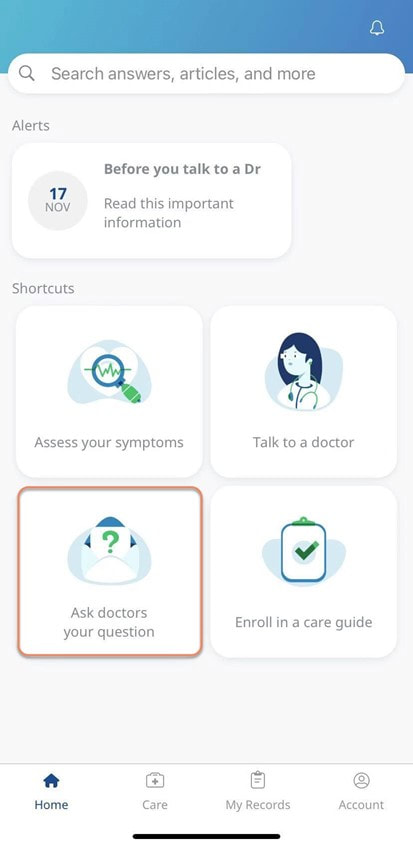
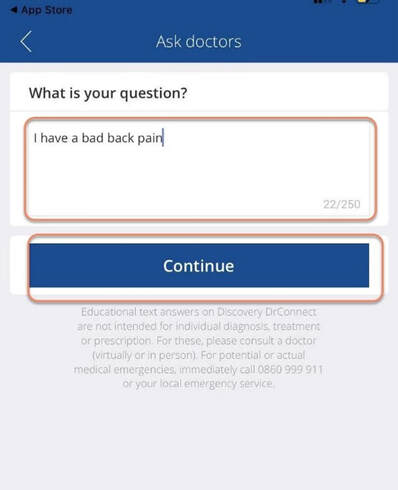
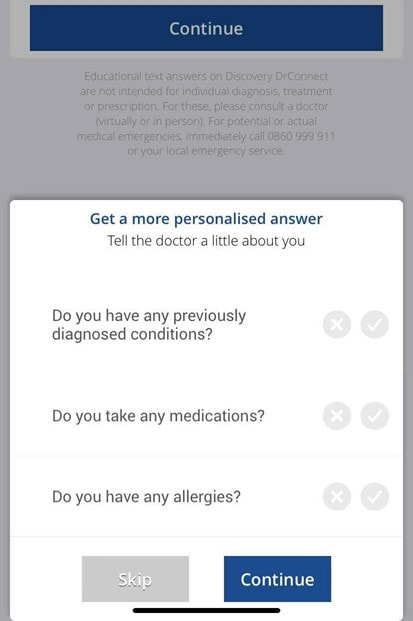
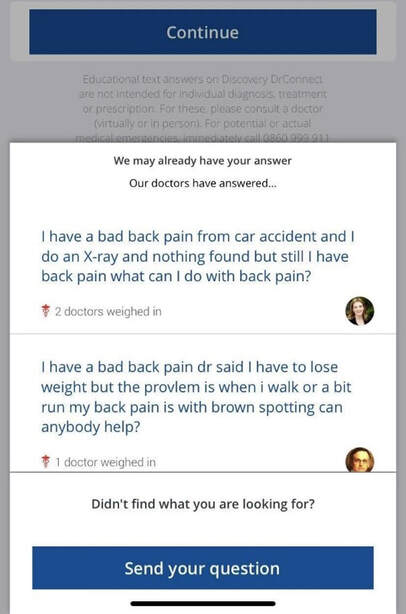
To help you stay healthy and informed on the COVID-19 situation, Discovery will continue to provide the most up-to-date information and guidance through COVID-19 Information Hub Below are Momentum Health Plan Guides Brochures for 2021 Below are Bonitas Plan Guides Brochures for 2021  Vitality is the world’s leading science-based behavioural-change programme that encourages and rewards you for living healthier, driving well and banking well. With over 10 million Vitality members in 22 markets enjoying thousands of rewards, you can be part of the Vitality family and start your journey to a healthier you and a safer way of life. Enjoy bigger, better rewards with Vitality. From half-price movies, flight savings, cash back on your groceries, fuel savings, weekly rewards and more, being healthier, driving well and banking well has never been more rewarding. The terms and conditions apply to the Vitality Premium Holiday special offer which gives eligible Discovery members by the Discovery Health, who join full Vitality Health or Vitality Purple between 01 October and 31 December 2020, the first three months of their membership free. For 1 November activation, the first premium will be deducted in February 2021; for 1 December activation, the first premium will be deducted in March 2021 and for 1 January activation, the first premium will be deducted in April 2021. For more information about the terms and conditions, please visit: https://www.discovery.co.za/assets/template-resources/terms-and-conditions/vitality/vitality-premium-holiday.pdf I have used up my Medical Savings Account, can I still see a doctor? I am a loyal customer of Discovery and have been a member of Discovery Health since I entered the workplace in 1996. During my start-up years from 2006 to 2009, I moved to my wife's company medical aid Sasolmed, then later changed to Medicover. In 2009, I returned to Discovery Health. My medical aid option has been Classic Delta Saver for the last few years. I think this plan is value for money, suitable for our family of five. However, towards the end of the year, I often run out of Medical Savings Account, then I have to pay out of my own pocket to see a doctor or to buy medicine. This plan provides Day-to-Day Extender Benefits: even when the savings account is used up, you can still visit a designated GP and be covered by Discovery. Discovery Health covers up to 6 network GP visits, which is helpful. The protocol to access this extender benefit has changed since the end of last year, however. Although I am a healthcare broker, I forgot to keep up with the change. I still wanted to use the same procedure as I have used in the past. I then ran into a wall and the Discovery Health refused to pay. What is going on here? There were like R30 left in my MSA. In order to use the extender benefits, I went to Dis-chem pharmacy to buy over-the-counter medicine. The intention was to reduce the savings account to zero. I asked the pharmacist to deduct from my savings account first, and I would pay the balance in cash. I also asked the pharmacist to confirm that there was no money in my savings account. After that, I made an appointment for my son with a designated family doctor, to assess his spinal injury. After the consultation, the front desk staff said that the claim had been submitted to Discovery Health, so I didn't have to pay for it. I thought that this extender benefit was really good, only to receive a claim statement from Discovery a few days later that they did not pay. I thought there was some misunderstanding. Upon further investigation, it turned out that I didn't apply the knowledge acquired. At the end of last year, Discovery announced a new process to use extender benefits. The first is to go to a network pharmacy such as Dis-chem to see a nurse. Or download the Dr Connect app on your mobile phone to consult with a doctor online. The infographic below illustrates: Below are the steps of how DrConnect works 1. Download DrConnect on the smart phone 2. Open the APP and log in 3. Log in with your Discovery Username and Password 4. You will see 4 categories: Assess your symptoms, Talk to a doctor, Ask doctors your questions, Enrol in a care guide. 5. If the GP you have visited before is also a DrConnect network doctor, he/she will appear here. Click the doctor for more options. 6. You can choose to book an appointment, send them a message about your queries, or connect for a video consultation (when they are online). 7. Or, on the main page (home), choose to ask a question. 8. Type in the question you would like to ask. 9. Answer a quick health survey or click Skip to skip it. 10. There may be other people have asked a similar question, which already has an answer to, see if you can find your answer here, if not, click to send your question.
It is now time to review your medical aid scheme cover for 2021. This means you have a window within which you can switch to a different plan for the new year. This window usually closes at the end of November (depending on your current provider), so don’t delay collecting the necessary information. This is not a decision to be rushed.
Why do I have to decide now? Medical aid providers allow you to switch to a higher plan once a year (at the end of the year) without penalties or consequences. If you want to save on premiums or you need to increase benefits, now is the time to do it. Generally, medical schemes give you until the end of the year to change your plan. What if I want to change providers altogether? If you are unhappy with your medical aid provider, you can switch to another at any time of the year. But before you do, consider the following: Waiting Periods Medical Aids by law must accept anyone who applies to join their scheme. To protect themselves from older or sickly members that join without having contributed to the risk pool, they usually impose a waiting period of between 3 and 12 months. Waiting periods will apply if 1) you have not been a member of another South African medical aid for the past three months or more, 2) if you change medical schemes before 2 years of being covered with your previous medical aid provider and 3) if you have a pre-existing medical condition. Finding out about any waiting periods is extremely important before deciding to change providers. Late joiner penalty As an additional means to manage the risk of older or sickly members joining without having contributed to the risk pool, medical schemes (according to the Medical Schemes Act) are entitles to add a late joiner penalty to your premium if you were not part of a medical scheme before 01 April 2001. The late joiner penalty is calculated (using a prescribed formula) based on the number of years that you were not on a registered South African medical scheme. The late joiner fee can range between 5% and 75% of the total contribution, depending on the number of years that you were not covered by a medical scheme. It is important to keep proof of all your previous medical scheme membership, as it would help reduce or remove the Late Joiner Penalty. General considerations When reviewing your medical aid plan, you should consider the following factors: - benefits - exclusions - co-payments and deductibles - provider network restrictions - financial soundness of the medical scheme - the medical scheme's service and ability to pay claims - premium (affordability) - gap cover product to supplement your medical aid. Please contact our health team, Tel 011-658-1333, Option 2, or email service@daberistic.com , to find out about different medical aid options. |
AuthorKevin Yeh Archives
January 2025
Categories
All
|
-
I would like to
- Signup Newsletter
- Schedule an appointment
- Go to hospital
- Deal with an accident
- Make a Claim
- Invest >
- Apply for insurance >
- Appoint Daberistic as broker
- Promotions >
- Update my policy >
- Make a Will
- Set up a business
- Get an accountant.
- Get business tax advice
- Get personal tax advice
- Preferred Suppliers >
- Cancel Daberistic Services
- Covid-19 toolkit
-
Invest
- Our fund selection process
- Retirement annuity
- Tax-free Investment Plan >
- Unit Trusts
- Guaranteed Investments >
- Preservation funds
- Offshore
- Education plan
- Endowment
- Participation Bond
- Deposits
- Business investment accounts
- Private investment accounts
- Exchange Traded Funds
- Share investing
- Personalised share portfolio
- Retirement income
- Retirement Funds
-
Health
- Life
- Insure
-
Financial Coach
-
Accounting & Tax
-
About us
-
我想要
- 财富管理
- 员工福利
- 人寿保险
- 医疗保险
- 财产险
- 会计师事务所
- 关于我们
-
I would like to
- Signup Newsletter
- Schedule an appointment
- Go to hospital
- Deal with an accident
- Make a Claim
- Invest >
- Apply for insurance >
- Appoint Daberistic as broker
- Promotions >
- Update my policy >
- Make a Will
- Set up a business
- Get an accountant.
- Get business tax advice
- Get personal tax advice
- Preferred Suppliers >
- Cancel Daberistic Services
- Covid-19 toolkit
-
Invest
- Our fund selection process
- Retirement annuity
- Tax-free Investment Plan >
- Unit Trusts
- Guaranteed Investments >
- Preservation funds
- Offshore
- Education plan
- Endowment
- Participation Bond
- Deposits
- Business investment accounts
- Private investment accounts
- Exchange Traded Funds
- Share investing
- Personalised share portfolio
- Retirement income
- Retirement Funds
-
Health
- Life
- Insure
-
Financial Coach
-
Accounting & Tax
-
About us
-
我想要
- 财富管理
- 员工福利
- 人寿保险
- 医疗保险
- 财产险
- 会计师事务所
- 关于我们
Services |
About us |
Support
|








 RSS Feed
RSS Feed