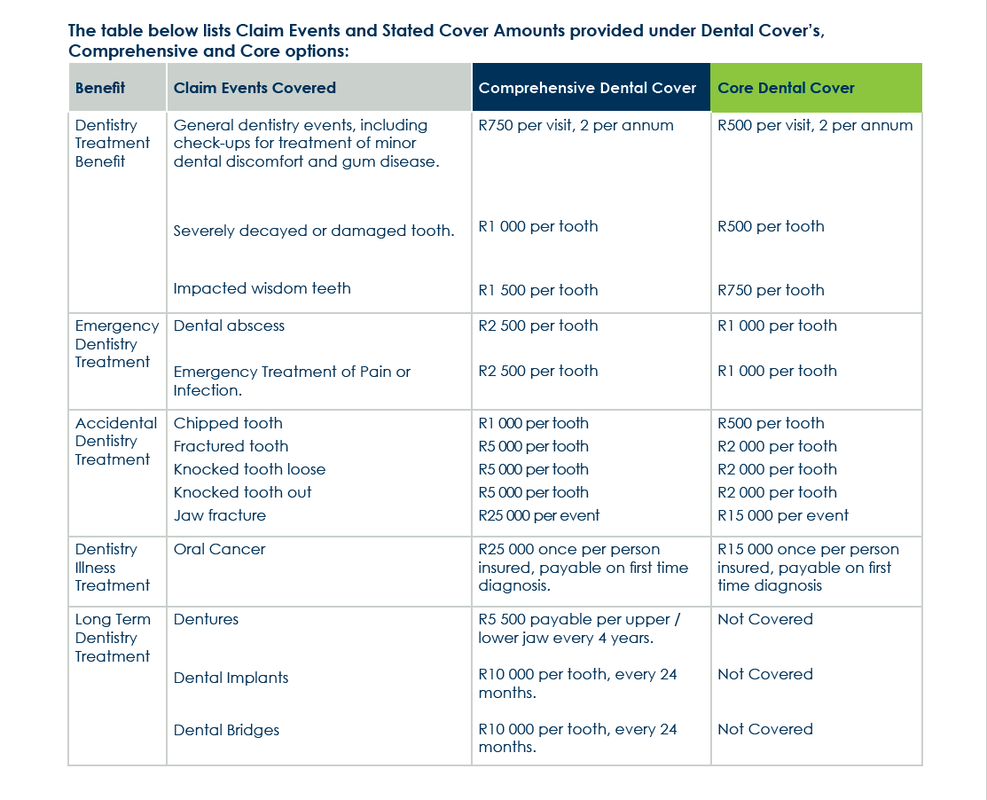
 Dentistry Cover is a health insurance policy that is designed to assist individuals and families to fund the high cost of private dentistry. Zestlife offers you a choice of Dentistry Cover options. Comprehensive Dentistry Cover: Provides funding for a comprehensive range of dentistry treatment costs. High stated cover amounts* are provided to fund in part or whole, the actual costs of dentistry, emergency, accidental, illness related and specialised dental treatment. Core Dentistry Cover: Provides more affordable funding for frequently incurred dentistry treatment costs. This option pays lower stated cover amounts* to fund in part or whole, the actual costs of dentistry, emergency, accidental and illness related dental treatment costs. The Comprehensive and Core options are suitable for individuals and families on medical aids that provide limited or no dental cover. Both the Comprehensive and Core options can also be used by individuals and families who are not on medical aid and have no existing dental cover. This is not a medical scheme and the cover is not the same as that of a medical scheme. This policy is not a substitute for medical scheme membership. *The stated benefit amounts are the total benefit to cover the costs relating to the diagnosis, subject to the terms and conditions of the policy. Who is covered? Cover is available to you as an “individual” as the only life insured or to you and your immediate family. The family option includes cover for yourself, spouse and children as well as grandchildren. To qualify for cover a grandchild must be a dependant on your medical aid. SPOUSE is the person to whom you are married by law, tribal custom or tenets of any religion and common law. Only one spouse can be covered under the policy. CHILD(REN) means your child or children, legally adopted children, stepchildren under the age of 21 or older if they are physically or mentally handicapped and dependant on the parents for financial support, or your grandchildren provided that they are dependants on your South African medical aid. If you would like to read more on this cover Click here
For a full consultation please contact Jo in our Health department email service@daberistic.com, tel (011)658-1333 Source: Zestlife
0 Comments
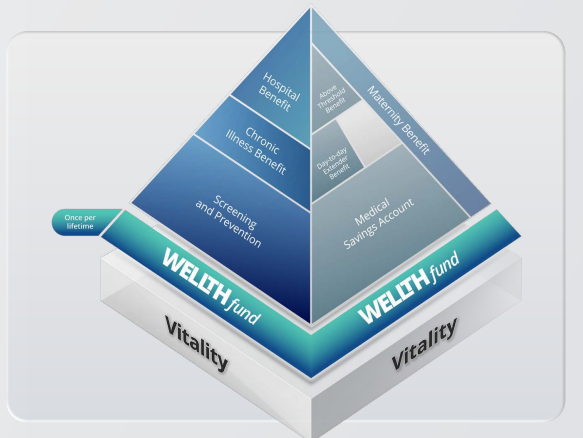
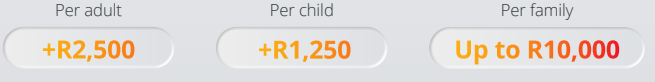
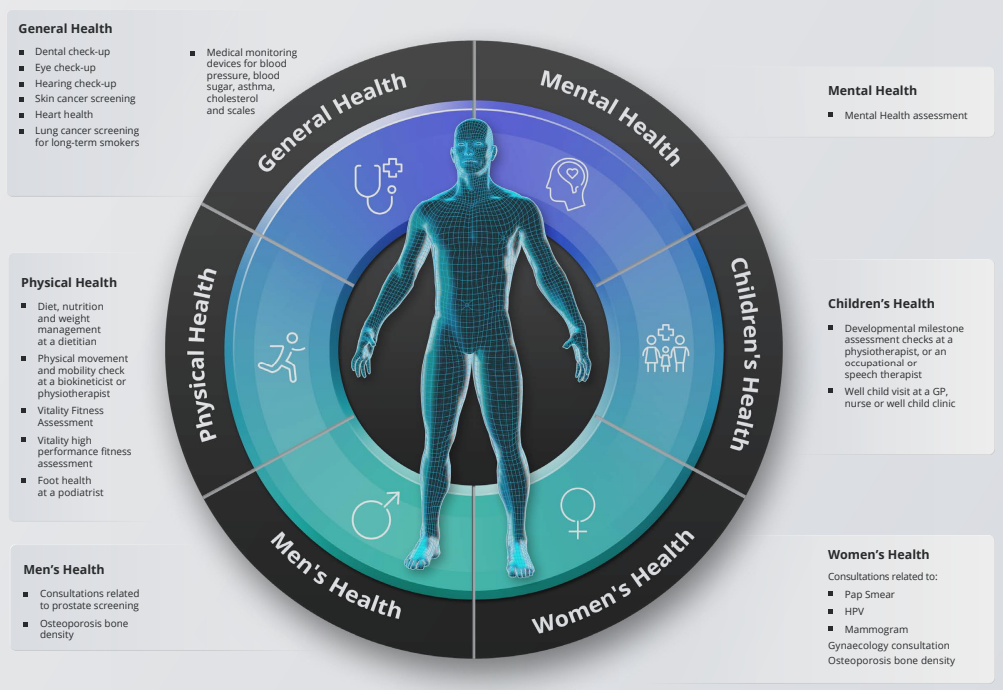
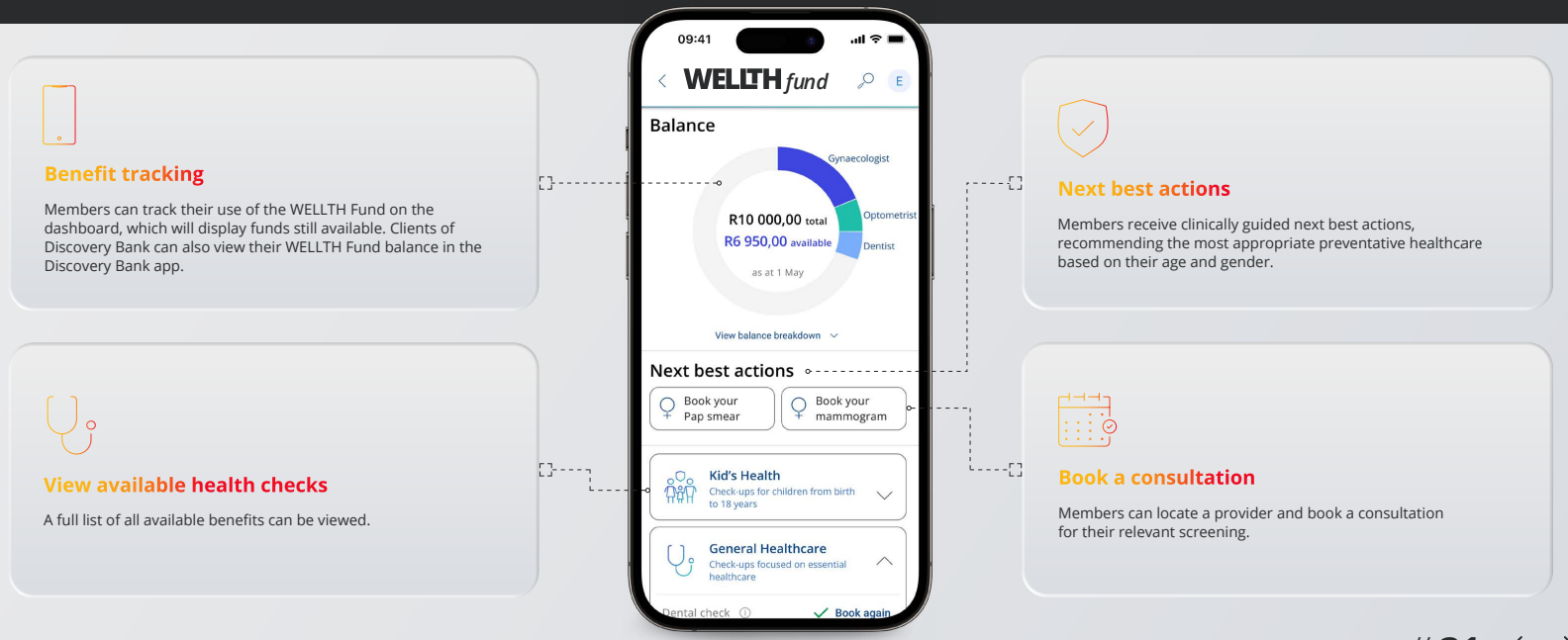
Discovery’s additional benefit the WELLTH fund came into effect on 01 January 2023. This benefit is a once-off benefit to all medical aid members in which it provides up to R10,000 in additional cover for a family’s healthcare needs. Fund Allocation The WELLTH Fund will be activated in 2023, once members completed their health check in 2022 or 2023 This sets the baseline for a member’s Health Status. To activate the WELLTH Fund, every person on a membership certificate aged 2+ must first complete their relevant health check at a healthcare provider in Discovery’s Wellness Network. Once the member and all their dependents have completed their Health Checks, they will have access to WELLTH Fund of up to R10,000, below is a chart of how funds are allocated. Where to use your WELLTH Fund The WELLTH Fund covers over and above the annual Screening and Prevention Benefit. Discovery App WELLTH fund tracking On your Discovery APP the WELLTH Fund Dashboard (shown below) will allow members to view all available health checks and recommended next best actions, book consultations and keep track of their use of the WELLTH Fund. How tests are covered
This benefit is available once per beneficiary, per lifetime. Discovery pays the above healthcare services from the WELLTH Fund up to the Scheme Rate and up to your WELLTH Fund limit. Some of these tests and treatments have a rand value limit depending on the number of active dependents you have on your membership. Once you have reached your allocated rand value limit for the tests, Discovery will pay any extra screening and preventive tests and treatments from your available day-to-day benefits, where applicable. The Scheme’s clinical entry criteria, treatment guidelines and protocols apply. The normal claims process applies. Discovery will automatically pay this from your WELLTH Fund. FAQ
Yes, the WELLTH Fund covers the following specific medical devices if they have a registered NAPPI code and are bought from a registered healthcare provider with a valid practice number (such as a pharmacy or doctor):
It depends on which health plan you have. Plan network rules apply for members on Smart and KeyCare plans:
Members on all other plans may use a provider of their choice and do not have to use a network provider to be covered by the WELLTH Fund. 4. The WELLTH Fund tool has recommended a list of check-ups that I should go for, am I only covered for these check-ups? No, the WELLTH Fund Tool is just a guide for which screening check-ups are most suitable for you, based on your age and gender. However, you can go for any of the screening and preventative check-ups covered by the WELLTH Fund - you don't have to go for those recommended by the tool. 5. Can I claim for medication from the WELLTH Fund? No, you cannot claim any medication from the WELLTH Fund. 6. How can I book an appointment to use my WELLTH Fund?
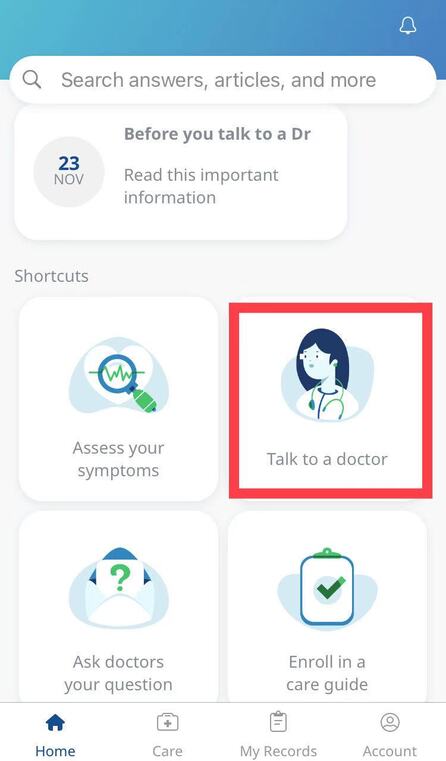
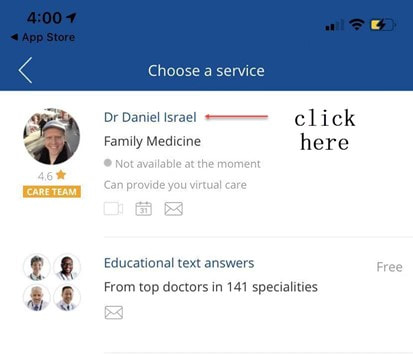
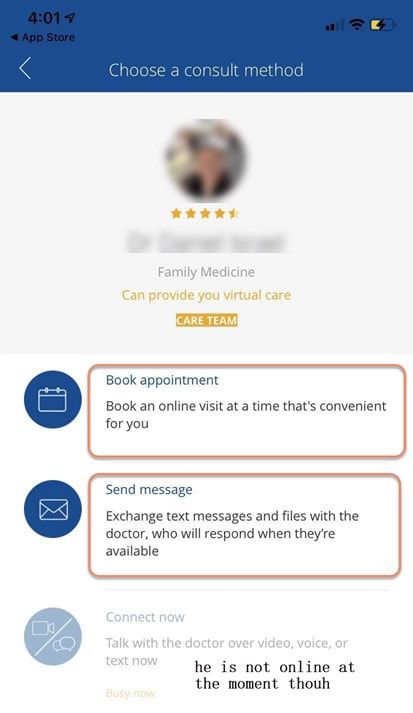
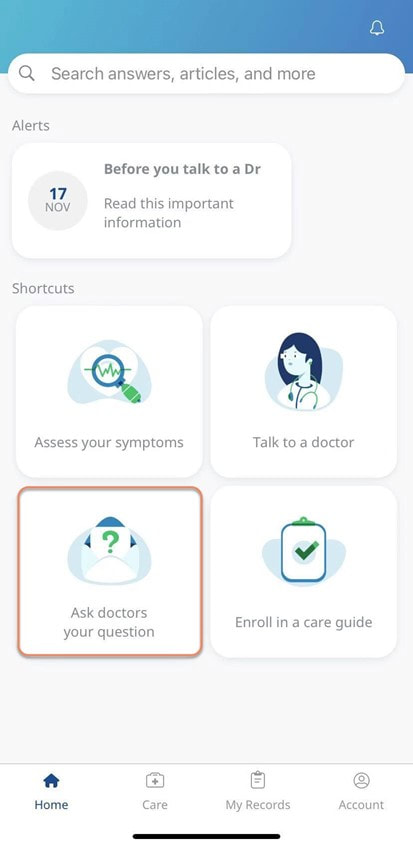
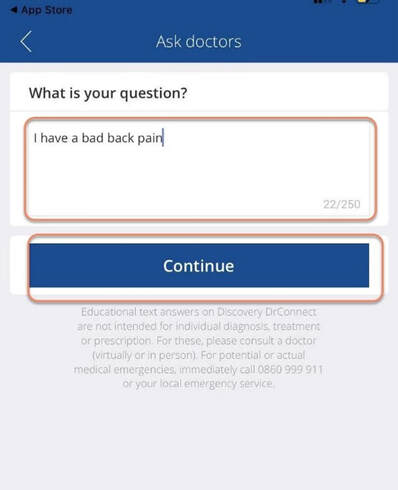
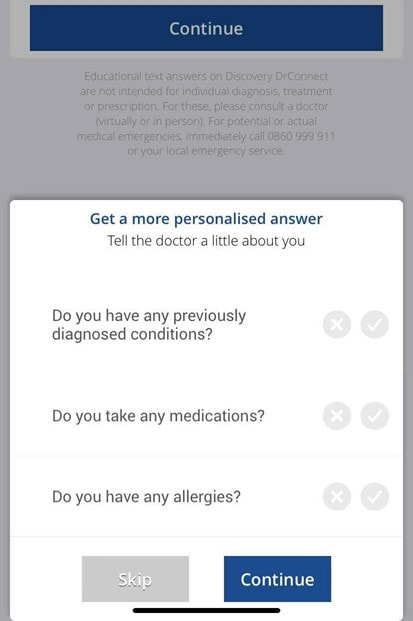
For more information, please contact our Health department on 011 658 1333 or email us on service@daberistic.com Source: Discovery  Vitality is the world’s leading science-based behavioural-change programme that encourages and rewards you for living healthier, driving well and banking well. With over 10 million Vitality members in 22 markets enjoying thousands of rewards, you can be part of the Vitality family and start your journey to a healthier you and a safer way of life. Enjoy bigger, better rewards with Vitality. From half-price movies, flight savings, cash back on your groceries, fuel savings, weekly rewards and more, being healthier, driving well and banking well has never been more rewarding. The terms and conditions apply to the Vitality Premium Holiday special offer which gives eligible Discovery members by the Discovery Health, who join full Vitality Health or Vitality Purple between 01 October and 31 December 2020, the first three months of their membership free. For 1 November activation, the first premium will be deducted in February 2021; for 1 December activation, the first premium will be deducted in March 2021 and for 1 January activation, the first premium will be deducted in April 2021. For more information about the terms and conditions, please visit: https://www.discovery.co.za/assets/template-resources/terms-and-conditions/vitality/vitality-premium-holiday.pdf I have used up my Medical Savings Account, can I still see a doctor? I am a loyal customer of Discovery and have been a member of Discovery Health since I entered the workplace in 1996. During my start-up years from 2006 to 2009, I moved to my wife's company medical aid Sasolmed, then later changed to Medicover. In 2009, I returned to Discovery Health. My medical aid option has been Classic Delta Saver for the last few years. I think this plan is value for money, suitable for our family of five. However, towards the end of the year, I often run out of Medical Savings Account, then I have to pay out of my own pocket to see a doctor or to buy medicine. This plan provides Day-to-Day Extender Benefits: even when the savings account is used up, you can still visit a designated GP and be covered by Discovery. Discovery Health covers up to 6 network GP visits, which is helpful. The protocol to access this extender benefit has changed since the end of last year, however. Although I am a healthcare broker, I forgot to keep up with the change. I still wanted to use the same procedure as I have used in the past. I then ran into a wall and the Discovery Health refused to pay. What is going on here? There were like R30 left in my MSA. In order to use the extender benefits, I went to Dis-chem pharmacy to buy over-the-counter medicine. The intention was to reduce the savings account to zero. I asked the pharmacist to deduct from my savings account first, and I would pay the balance in cash. I also asked the pharmacist to confirm that there was no money in my savings account. After that, I made an appointment for my son with a designated family doctor, to assess his spinal injury. After the consultation, the front desk staff said that the claim had been submitted to Discovery Health, so I didn't have to pay for it. I thought that this extender benefit was really good, only to receive a claim statement from Discovery a few days later that they did not pay. I thought there was some misunderstanding. Upon further investigation, it turned out that I didn't apply the knowledge acquired. At the end of last year, Discovery announced a new process to use extender benefits. The first is to go to a network pharmacy such as Dis-chem to see a nurse. Or download the Dr Connect app on your mobile phone to consult with a doctor online. The infographic below illustrates: Below are the steps of how DrConnect works 1. Download DrConnect on the smart phone 2. Open the APP and log in 3. Log in with your Discovery Username and Password 4. You will see 4 categories: Assess your symptoms, Talk to a doctor, Ask doctors your questions, Enrol in a care guide. 5. If the GP you have visited before is also a DrConnect network doctor, he/she will appear here. Click the doctor for more options. 6. You can choose to book an appointment, send them a message about your queries, or connect for a video consultation (when they are online). 7. Or, on the main page (home), choose to ask a question. 8. Type in the question you would like to ask. 9. Answer a quick health survey or click Skip to skip it. 10. There may be other people have asked a similar question, which already has an answer to, see if you can find your answer here, if not, click to send your question.
Momentum Medical Scheme focuses more than ever on keeping benefit design stable and ensuring that their members continue to enjoy comprehensive and affordable benefits. The 3rd largest open medical aid scheme in South Africa, Momentum Medical Scheme has announced an average annual contribution increase of 3.9% for 2021. This is substantially lower that the weighted average annual contribution increase of 8.2% for 2020.
If you have any queries or are interested in joining Momentum Medical Scheme, please contact us on 011-658-1333, 076-200-5488 or email service@daberistic.com. Discovery continues to lead the industry by rolling out exciting benefits and offerings: Mental wellbeing Shari'ah compliance arrangement Infertility and assisted reproductive therapy benefit Hospital network and day surgery updates New clinic and other services for employers Diabetes care programme Chronic Illness Benefits Co-payments and deductibles To find out more, please click on each tab below.
<
>
Mental wellbeing Statistics according to WHO shows one in four people in the world will be affected by mental disorders at some point in their lives, this positions mental disorder amongst one of the leading causes of ill-health worldwide. Mental ill-ness often left undiagnosed and with 84% of adults never receiving treatment and this impacts society and WHO estimates cost to global economy may exceed $16 trillion by 2030. Discovery’s approach to alleviate this disorder, they have introduced management in mental wellbeing. Below programs offered are:
Shari’ah compliant arrangement From 2021 members from our Muslim community can appoint to have their contribution and claims across all plans to conform with Shari’ah principles through the Shari’ah compliant arrangement. • Model is compliant and is based on Takaful principles • Process flow happens in an acceptable manner • No interest earned or paid at any stage • No ambiguity in contracts • Members’ interests are protected • Investments are managed in Shari’ah Compliant manner • No interest earned or paid on Shari’ah Compliant arrangement. Funds will be invested in a compliant manner allowing members opportunity to earn profit on Medical Savings Account balances. • Members that partake in this arrangement attain affirmation on their contribution and balances remaining after settlement of claims and other expenditure will be invested in Shari’ah compliant investments. Infertility and assisted reproductive Therapy benefit When a couple is looking forward to building a family and the incapability to fall pregnant is aggravating. It affects many families and takes a emotional toll, however, many infertility cases can be remedied through treatment such as drug, surgical repair and assisted reproductive techniques including intra-urine insemination (IUI) and in vitro fertilisation (IVF). Taking a leap of faith on possibility to become a parent can come with a price tag, an average of R65000.00 – R85000.00 for a single IVF treatment cycle, this may be a hefty cost for many families in which will hinder and or have reservations from taking on this treatment. Discovery would like to support couples/ families distressed from infertility with introducing cover for Assisted Reproductive Technologies (ART) and the benefit will include cover for: • Up to two cycles of ART if Scheme’s benefit and clinical entry criteria are met. • This includes a series of care for the progress of the full duration: consultations, ultrasounds, oocyte retrieval, embryo transfers, admission costs including lab fees, medication and embryo and sperm storage. • The total limit of R110 000.00 per person per year at Discovery health rate applies. • Members will be subject to 25% of the costs and any excess above the Discovery Health Rate. • This benefit will be attainable at Southern African Society of Reproductive Medicine and Gynaecological Endoscopy (SASREG) accredited centres only and subject to clinical pathways and protocols. • Lastly, the benefit is only available to female members that has been on Executive and Comprehensive Plans for at least 2 years and the age between 25-42 years old.
<
>
Chronic Illness Benefits
Diabetes Care Programme 2021 Premier Plus GP network will become the Designated service provider for members with Diabetes on the comprehensive plans. It is supported by the extensive coverage offered by the Premier Plus GP network and the clinical outcomes achieved by the diabetes care programme. The chosen GP will be member’s DSP for the ongoing management of diabetes as well as cardiovascular conditions. Statistics has shown in improvement when member’s care is coordinated by a single doctor. Hospital Network Updates and Day Surgery New hospitals will be added, and some existing hospitals will be replaced with region specific substitutions for 2021 to ensure continued optimisation of the Delta, Smart and KeyCare hospital networks In the Day Surgery, they will extend this offer to Comprehensive plans given focus on provider and patient safety because of COVID-19. The 2021 new hospital network and day surgery lists will be published by the end of October 2020.
<
>
Limits, Co-payments, deductible and Thresholds
Next: Vitality 2021 - To Help members stay motivated Co-payments For Endoscopic Procedures
New Clinic and Other Services for Employers Daily monitoring of COVID-19 exposure, prevalence, and disease progression:
Medical aid is a necessary yet expensive purchase in South Africa. Due to the public healthcare system unable to cope with the public demand, people who can afford it or who work for larger employers will choose private healthcare. They buy medical scheme products to cover such healthcare expenses.
Since medical aid is expensive, it is important for a member to understand its benefits, in order to make the best use of it when needed. As each new year begins medical aid members start with a clean slate, with new benefits and replenished savings available. If you manage your medical expenses correctly you can avoid out-of-pocket expenses and limit the possibility of running out of benefits. 1. Read up on your medical aid plan Take the responsibility of understanding your medical aid plan. Visit the medical scheme's website, find your specific medical aid plan information and read through it. Check out the FAQs. If your medical scheme creates YouTube videos on your specific plan and benefits, watch these videos. The more you understand your medical aid plan, the better you are in a position of making use of benefits provided for by the plan. 2. Speak to your Healthcare Advisor Medical aid plans are complex. A medical aid plan has many details, terms and conditions. Many members will struggle to make sense of it. A Healthcare Advisor with suitable qualification, training and years of experience can simplify matters for you and answer your specific questions. 3. Find a GP on your medical aid's network Using network doctors is an invaluable tool to make your medical aid last longer as it means you won’t be charged more than a specific amount. 4. Always use partner networks Medical schemes negotiate preferential rates with providers who have partnered with them. This means if you use a network hospital, doctor or pharmacy you will not be charged more than the rate agreed with the scheme. This will also help you to avoid co-payments, deductibles and additional out-of-pocket expenses. 5. Ask your pharmacist Buy over-the-counter medicine to treat less serious ailments and consider using generic medicine which is cheaper but effective. Pharmacists are able to provide sound medical advice on problems such as rashes, colds or illnesses that are not severe, simply ask! 6. Going to hospital - get the facts Talk to your doctor or specialist before being admitted to hospital. Check what they are going to be charging and what your scheme will cover. If there is a large difference, don’t be afraid to approach your doctor to see if they are prepared to adjust their fee. Alternatively, you can also check if there are other healthcare providers who are on your scheme’s network that will charge you a better rate. 7. Remember to pre-authorise Pre-authorisation is required for all hospital admissions to ensure your stay will be covered. Always ask if there are any co-payments or sub-limits that will apply and what you can do to avoid these. For planned procedures, it’s also worth checking with your scheme if you will obtain better cover by using contracted providers or having the procedure performed in the doctor’s rooms or a day clinic. 8. ICD-10 codes If you need to undergo an operation, ask your surgeon for the codes that will be charged. This will include the procedure codes and those for any other products that will be needed, this all helps with pre-authorisation and ensuring the costs will be covered. 9. Chronic health conditions Some schemes offer programmes to help you manage severe chronic conditions such as cancer, diabetes and HIV/AIDS. These programmes are usually covered from the risk portion of your medical contribution and are not funded from your savings account. They help you use your benefits to maximum advantage while ensuring you receive quality care by using specific providers. With thanks to: www.w24.co.za |
AuthorKevin Yeh Archives
January 2025
Categories
All
|
-
I would like to
- Signup Newsletter
- Schedule an appointment
- Go to hospital
- Deal with an accident
- Make a Claim
- Invest >
- Apply for insurance >
- Appoint Daberistic as broker
- Promotions >
- Update my policy >
- Make a Will
- Set up a business
- Get an accountant.
- Get business tax advice
- Get personal tax advice
- Preferred Suppliers >
- Cancel Daberistic Services
- Covid-19 toolkit
-
Invest
- Our fund selection process
- Retirement annuity
- Tax-free Investment Plan >
- Unit Trusts
- Guaranteed Investments >
- Preservation funds
- Offshore
- Education plan
- Endowment
- Participation Bond
- Deposits
- Business investment accounts
- Private investment accounts
- Exchange Traded Funds
- Share investing
- Personalised share portfolio
- Retirement income
- Retirement Funds
-
Health
- Life
- Insure
-
Financial Coach
-
Accounting & Tax
-
About us
-
我想要
- 财富管理
- 员工福利
- 人寿保险
- 医疗保险
- 财产险
- 会计师事务所
- 关于我们
-
I would like to
- Signup Newsletter
- Schedule an appointment
- Go to hospital
- Deal with an accident
- Make a Claim
- Invest >
- Apply for insurance >
- Appoint Daberistic as broker
- Promotions >
- Update my policy >
- Make a Will
- Set up a business
- Get an accountant.
- Get business tax advice
- Get personal tax advice
- Preferred Suppliers >
- Cancel Daberistic Services
- Covid-19 toolkit
-
Invest
- Our fund selection process
- Retirement annuity
- Tax-free Investment Plan >
- Unit Trusts
- Guaranteed Investments >
- Preservation funds
- Offshore
- Education plan
- Endowment
- Participation Bond
- Deposits
- Business investment accounts
- Private investment accounts
- Exchange Traded Funds
- Share investing
- Personalised share portfolio
- Retirement income
- Retirement Funds
-
Health
- Life
- Insure
-
Financial Coach
-
Accounting & Tax
-
About us
-
我想要
- 财富管理
- 员工福利
- 人寿保险
- 医疗保险
- 财产险
- 会计师事务所
- 关于我们
Services |
About us |
Support
|







 RSS Feed
RSS Feed