|
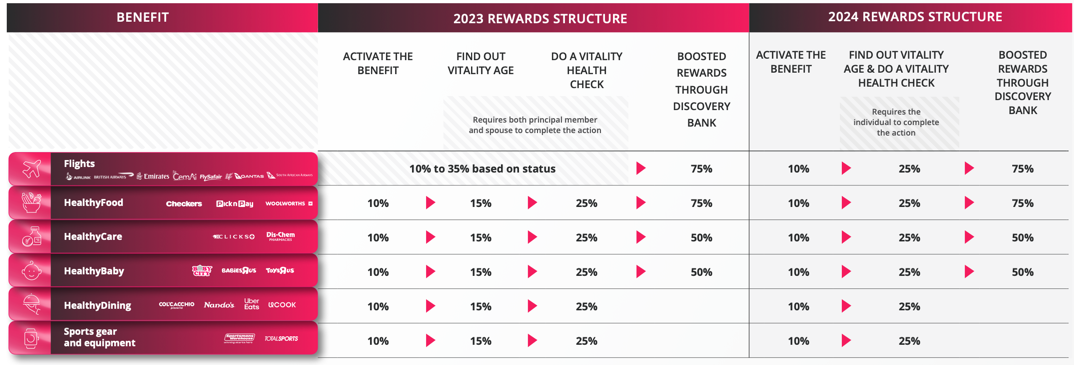
Vitality is the largest wellness programme in South Africa, as well as globally. It helps members know their health, improve their health and enjoy rewards. Here are the highlights of the 2024 update: 1. The next evolution of HealthyFood Since its introduction to the Vitality programme in 2009, the Vitality HealthyFood benefit has succeeded in making healthy choices more affordable, driving behaviour change and ultimately resulting in better health outcomes for members. Vitality HealthyFood is a benefit loved and used by members. The most popular food items purchased are: Bananas (3.6 million bags) Potatos (3.1 million bags) Cucumber (2.8 million) Grocery delivery has become increasingly popular with South African households since the COVID-19 pandemic, becoming a part of the weekly routine for many and influencing the choice of preferred grocery retailer. In 2024, it's enhancing the benefit by introducing Checkers as a new Vitality HealthyFood partner. Checkers' home delivery service, Sixty60, has already become a household brand. It will go live on Vitality in the second half of 2024. Plus, it's revamping the benefit by offering members the choice of an in-store and online grocery partner. For example, a member can choose Woolworths as the Primary in-store partner and Checkers as the Primary online grocery partner. 2. Exercise anywhere with Vitality Fitness For over 25 years, Vitality’s fitness benefits have driven hundreds of thousands of Vitality members to get healthier and rewarded. From 2024, we’re addressing individual exercise needs with Vitality Fitness – a first-of-its-kind integrated exercise ecosystem. Through Vitality Fitness, members can now access a variety of exercise opportunities at the gym and beyond. This includes combat sports, CrossFit, dance, HIIT, pilates, padel, yoga. 3. Encouraging engagement with the Vitality Health Check The Vitality Health Check gives Vitality members a valuable snapshot of their health status. By completing a Vitality Health Check, members can detect lifestyle-related diseases early and manage their health risks with tailored interventions. In 2024, the Vitality Health Check becomes more valuable than ever before, with discount structures and Vitality points being adjusted accordingly. All rewards including flights, HealthyFood, HealthyCare, Sports gear and equipment require an annual VItality Health Check to increase the discount to 25%. 4. Introducing a new measure of cardio fitness to the Vitality programme
Cardio fitness is a measure of how well the respiratory and circulatory system supply oxygen during sustained periods of physical activity. The most reliable and valid measure of cardio fitness is VO2 max. From next year, members will earn up to 10,000 Vitality points based on their VO2 max estimates measured on their Apple, Garmin or Samsung fitness device. 5. Improving the experience for new Vitality member From December 2023, new Discovery Health Medical Scheme members who have signed up for Vitality will have immediate access to Vitality benefits and rewards and no longer have to wait until the start date of their health policy. New Discovery Health Medical Scheme members joining Vitality get to enjoy Vitality for free from the month they join, as well as the following 2 months. 2024 Vitality premium: Single R359 M+1 R439 M+2+ R509
0 Comments
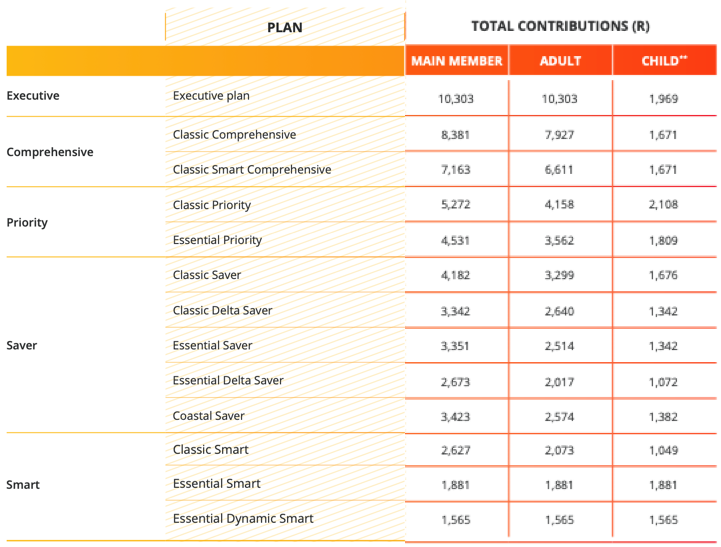
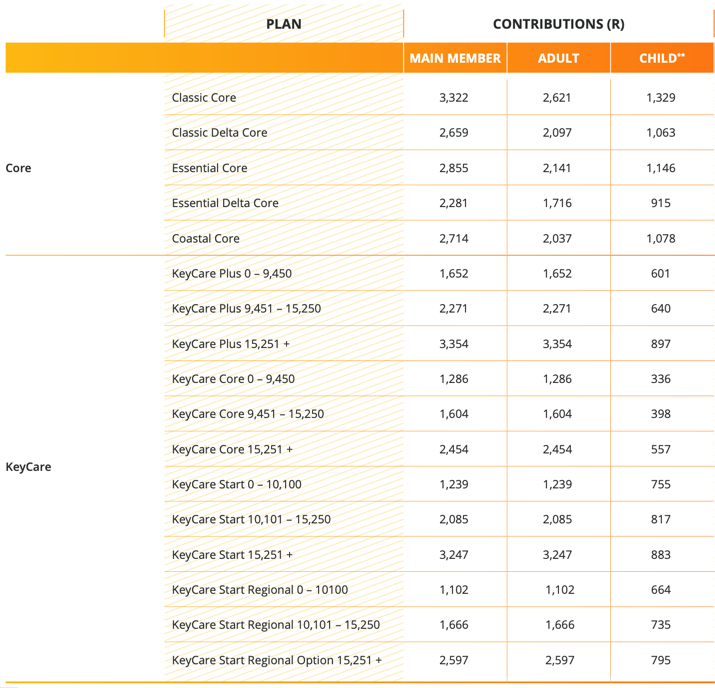
On the 26th of September, Discovery announced its Discovery Health update for 2024. Below are the highlights: 1. Transforming members’ healthcare experience with the new Discovery Health app Your gateway to a personalised, end-to- end healthcare journey. Conveniently access care and manage your health and health plan benefits in a single app. The new app also enables new benefits for all members of Discovery Health Medical Scheme including Virtual Urgent Care, Virtual Physical Therapy, the Mental Health Assessment Benefit and digital therapeutics for mental health. You can already download the app from the App Store and Google Play. 2. Balancing affordability, sustainability and value for members in 2024 and beyond Increases to contributions for 2024 will be plan specific and will range from 0% to 12.9%, to maintain contributions in line with expected claims experience, while supporting affordability for members. Targeted plan and benefit updates for the Comprehensive series and KeyCare series ensures long-term sustainability of the benefits offered by these plans. The Comprehensive series currently has five plans. It will be consolidated into two options in 2024: Classic Comprehensive and Classic Smart Comprehensive. 3. Creating personal health pathways for all members In 2024, all Discovery Health Medical Scheme members will have access to a personal health pathway that predicts the most important actions they can take to improve their health. Members are encouraged to complete actions through an intelligent, gamified experience, which has been personalised for every adult member on the Scheme. 4. Expanding access to healthcare cover with Flexicare Flexicare is a health insurance product designed to provide a wide range of day-to-day healthcare benefits with optional add-ons, such as such as unlimited GP consultations, medicine, dentistry, optometry and so much more. Flexicare will be enhancing its primary healthcare offering in 2024 to include a nurse-led clinic pathway that provides increased access to quality primary healthcare at an affordable price point. The 2024 Discovey Health contribution table is as follows: The most affordable medical aid plan independent of income is Essential Dynamic Smart, R1,565 per month.
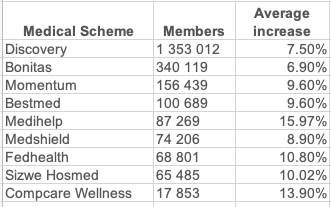
The most expensive plan, which provides the most comprehensive benefits, is the Executive Plan, which costs R10,303 per month. If you want to get or review the medical aid for your employees, please call our Health Department on 011-658-1333 or email service@daberistic.com. All the large open medical schemes in South Africa have announced their contribution increases for 2024. Below is the list. Discovery Health says the average weighted increase across DHMS plans is 7.5% for 2024. Excluding the Medical Savings Accounts, the increase on Risk Contributions is 10.5%.
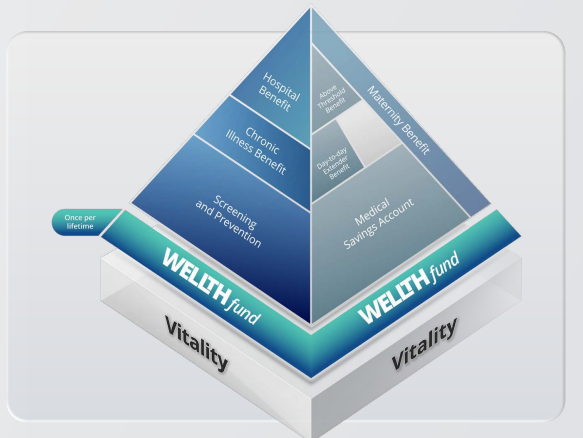
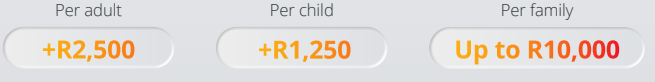
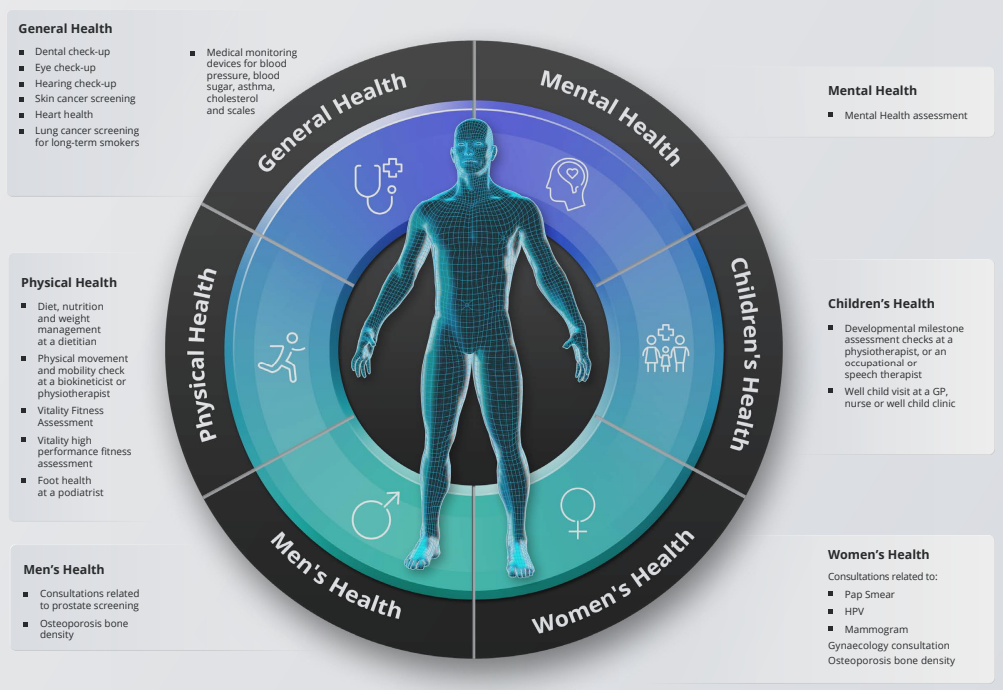
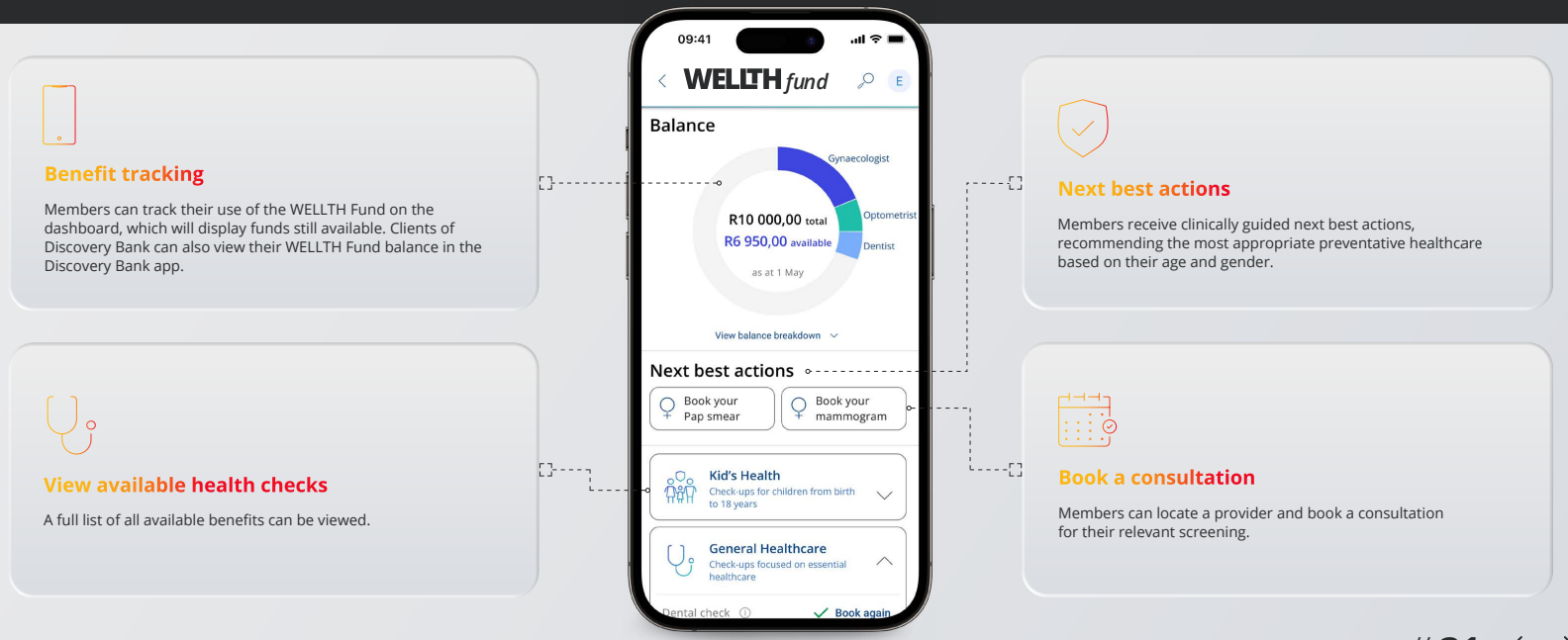
If you want to review your medical aid plan, please call our Health Department on 011-658-1333, Option 2 or email service@daberistic.com. Discovery’s additional benefit the WELLTH fund came into effect on 01 January 2023. This benefit is a once-off benefit to all medical aid members in which it provides up to R10,000 in additional cover for a family’s healthcare needs. Fund Allocation The WELLTH Fund will be activated in 2023, once members completed their health check in 2022 or 2023 This sets the baseline for a member’s Health Status. To activate the WELLTH Fund, every person on a membership certificate aged 2+ must first complete their relevant health check at a healthcare provider in Discovery’s Wellness Network. Once the member and all their dependents have completed their Health Checks, they will have access to WELLTH Fund of up to R10,000, below is a chart of how funds are allocated. Where to use your WELLTH Fund The WELLTH Fund covers over and above the annual Screening and Prevention Benefit. Discovery App WELLTH fund tracking On your Discovery APP the WELLTH Fund Dashboard (shown below) will allow members to view all available health checks and recommended next best actions, book consultations and keep track of their use of the WELLTH Fund. How tests are covered
This benefit is available once per beneficiary, per lifetime. Discovery pays the above healthcare services from the WELLTH Fund up to the Scheme Rate and up to your WELLTH Fund limit. Some of these tests and treatments have a rand value limit depending on the number of active dependents you have on your membership. Once you have reached your allocated rand value limit for the tests, Discovery will pay any extra screening and preventive tests and treatments from your available day-to-day benefits, where applicable. The Scheme’s clinical entry criteria, treatment guidelines and protocols apply. The normal claims process applies. Discovery will automatically pay this from your WELLTH Fund. FAQ
Yes, the WELLTH Fund covers the following specific medical devices if they have a registered NAPPI code and are bought from a registered healthcare provider with a valid practice number (such as a pharmacy or doctor):
It depends on which health plan you have. Plan network rules apply for members on Smart and KeyCare plans:
Members on all other plans may use a provider of their choice and do not have to use a network provider to be covered by the WELLTH Fund. 4. The WELLTH Fund tool has recommended a list of check-ups that I should go for, am I only covered for these check-ups? No, the WELLTH Fund Tool is just a guide for which screening check-ups are most suitable for you, based on your age and gender. However, you can go for any of the screening and preventative check-ups covered by the WELLTH Fund - you don't have to go for those recommended by the tool. 5. Can I claim for medication from the WELLTH Fund? No, you cannot claim any medication from the WELLTH Fund. 6. How can I book an appointment to use my WELLTH Fund?
For more information, please contact our Health department on 011 658 1333 or email us on service@daberistic.com Source: Discovery  All Medical aid Options would include: Accidental or emergency medical hospitalisation, maternity benefits, chronic illness benefits, oncology benefits, mammogram screening (once every 2 years), pap smear screening (once every 3 years), and prostate cancer screening (once a year). Below we detail each cover and how it works. Hospitalisation Whether your medical aid option is a hospital plan or a savers plan, as long as you are hospitalized in South Africa and obtain the hospitalization pre-authorization, you are covered. In case of emergency hospitalization, the hospital will contact the Medical aid company directly and obtain authorization When hospitalized, the hospital bill and the doctors’ bills are separate. In the case of elective hospitalization (planned procedure), the Medical Aid company will pay the hospital bill in full (in most of the cases). In terms of doctor's fees, medical aid company will pay according to the scheme rate. For example, if the scheme rate for a certain operation is R5,000, but the doctor can decide how much to charge. If the doctor charges R15,000, the Medical Aid company will only pay R5,000, and the remaining R10,000 is your liability. If you have Gap Cover, the the co-payment can be claimed back. If the patient is hospitalized due to an accident, an emergency or critical illness (such as cerebral hemorrhage), the doctor does not charge more than scheme rate, and the Medical Aid company will pay for the medical cost, and this is unlimited. In addition to applying for pre-authorization for hospitalization, you can also apply for pre-authorization with the Medical Aid company if you need to do endoscopy (as out-of-hospital) so that the Medical Aid company will settle the medical expenses. It should be noted that if your endoscopy is done in a hospital or a day hospital, you will need to pay a co-payment; If it is done in the doctor's room, there won’t be a co-payment. What should you do if the doctor asks you to request for pre-authorization? You need to ask the doctor for the following information and provide it to the Medical Aid company: • Medical aid membership number • Name the patient • Reasons for hospitalization or surgical items • Date and time of admission • Name and practice number of doctor • Hospital name and practice number • ICD10 codes and procedure codes Maternity Benefit If you have confirmed your pregnancy with your doctor, you can activate the maternity benefits with the Medical Aid company. After that, your medical aid would compensate 8 maternity check-ups up to scheme rate (about R480). Each obstetrician and gynecologists' charges different fees, you will then need to pay the amount exceeding the scheme rate. If your Gap Cover is with Sirago Ultimate option, 4 out of the 8 times, you may claim back the difference paid. Chronic Benefit If you are diagnosed with chronic illness, you can ask your medical aid broker for a chronic illness benefit application form, and ask your doctor to fill it out and send it to the Medical Aid company (or send it to the broker, who will send it to the Medical Aid company). In this way, you can go to the pharmacy for medicine every month, and the Medical Aid company will pay for the medicine. Cancer If you are diagnosed with cancer, you need your oncologist to provide a treatment plan and histology report to the Medical Aid company. Once the oncology benefit is activated, the first R200k of each cycle (12 months) will be paid in full, up to scheme rate. After that, Medical Aid company will pay 80%, and the remaining 20% will be your own expense. (if you have Gap Cover, the 20% co-payment amount can be claimed back) If your Gap Cover is Sirago's Ultimate option, the Gap cover will also compensate you R25k. Day-to-day Medical Expenses - Medical Savings If you are on a Savers option (or higher), you can enjoy day-to-day benefits. Every January, Discovery gives you your full-year savings which you may use throughout the year, if the savings are not used up by the end of the year, it gets rolled over to the next year and you can accumulate it and earn interest. If you are on a Priority, Comprehensive, or Executive plan, you also enjoy the Above Threshold Benefits, given that you have paid up the Self Payment Gap. What can you use Medical Savings for? You can use your Medical Savings for any out-of-hospital medical-related expenses, including but not limited to doctors' consultations, over-the-counter medication, dentists, glasses, certain co-payments (scopes, out-of-hospital CT/MRI scans), etc. Once the savings are used up, you will then need to pay for the medical expenses from your own pocket, until January the following year. Written by: Tammy Hua If you would like to review your Medical Aid option contact Tammy email: service@daberistic.com (tel)11)658-1333 Ext 106  Due to pandemic, rising costs and high taxes are eroding pensions and retirement savings in South Africa. Many are forced to use the state-funded healthcare services which is already under pressure, causing long queues and even longer waiting lists. There is no doubt that we want the best medical attention for our elderly parents when they fall ill therefore private health care is our solution. It is important to understand what options is best suited for your aging parent’s needs. Where do you start? You would need to sit down and discuss with your parents and obtain the following information:
Once you have answers to the above, the next set of questions you need to discuss is to do a realistic budget to finance the plan.
What if your parents cannot contribute? If your aging parents are financially dependent on you and you happen to be main member of a medical aid policy, you may consider adding them as your dependent as this means they can pay a reduced rate. However, they will be on the same option plan as you, should your option not be sufficient to cover their needs, your option is to upgrade your plan. If you’re on an option that includes savings, they become eligible for using your savings. You will need to be prepared for savings being exhausted due to extensive care required. What happens when parents don’t qualify as your dependent? If you decide to not add parents as Dependants or due to parents not qualifying to be your dependent, they can always choose a medical option according to budget and below are things to consider for when choosing your option. Full medical cover (with savings): On a comprehensive option, most elements are covered for. Such as hospital admission, chronic medication and day to day expenses, medical equipment, and possibly dentistry and optometry. These plans vary widely therefore, read through entire plan before signing up to make sure it qualifies all your parent’s needs. Basic hospital plan: These covers around 90% of hospital procedures, basic prescribed minimum benefit (PMB) condition and cancer benefit. It excludes expenses such as none PMB approved medication, equipment, doctor’s visits, optometry, or dentistry. This may not be a full coverage but highly affordable option. Gap cover is always recommended by Daberistic as this boosts your unforeseen gap payment by 500%. To read more about gap cover click here. What else to keep in mind?
If you would like cover for your parents, please contact Namhla or Tammy in our health department, email Service@daberistic.com, Tel 011-658 1333, option 2 for Medical Aid.  When to take a test and when will it get covered? You’re covered for 2 COVID-19 Polymerase Chain Reaction (PCR) screening tests every calendar year (1 January to 31 December), regardless of the outcome of the test. Medical Aid will pay for COVID-19 diagnostic tests, provided that the member who took the test:
Will you have to pay upfront and submit a claim for it to be paid from this benefit? This depends on the payment arrangements your medical aid have with your healthcare provider. If your healthcare provider submits a claim on your behalf, your medical aid will reimburse them directly subject to meeting the clinical entry criteria of the benefit. If your doctor requires you to pay upfront, you can submit your claim to your medical aid. What does it mean if I test positive for the PCR test? A positive PCR result confirms that you are infected and that you can spread it to others. You would need to contact your doctor to discuss the implications of this finding and the next steps to take, whether this be to self-isolate at home and/or on your planned hospital admission. If I test Positive, how do I self-isolate and for how long do I self-isolate? If you are infected and are asymptomatic i.e. you show no symptoms, you must stay at home and self-isolate for 10 days from the date of your positive test. In case of severe respiratory illness or severe shortness of breath you need to immediately consult with your doctor or go to the nearest hospital emergency unit. In case of severe disease, you will probably be hospitalised, and you would need to continue to self-isolate for 10 days after clinical stability is achieved. If I test positive for Antibody test, will I have immunity to COVID-19 infections in the future? As COVID-19 is a new virus, we cannot tell for sure how long antibodies will last or how well they can protect against future infections. Even though it is believed that a person will have some level of immunity after infection, which is the scientific principle that the development of a vaccine is based on. However, all individuals should still adhere to recommendations by the department of health on social distancing, hygiene, and personal protection, regardless of their antibody test result. How am I covered for COVID-19? This benefit, available on all plans, is covered by the scheme for cases of outbreak diseases and out of hospital healthcare services related to COVID-19. These healthcare services are covered up to maximum of 100% of your chosen medical scheme’s rate in accordance with Prescribed minimum benefits where applicable. Am I covered if I am in a waiting period? The scheme resolved to change its’ approach to underwriting for the duration of the outbreak, specifically with regards to cover for COVID-19. Members that are diagnosed with COVID-19 after joining will have access to the benefit, even if they are subject to a waiting period at the time of being diagnosed with COVID-19. Members that are diagnosed with COVID-19 before joining the scheme will not have access to the benefit and will be subject to waiting period to protect the scheme and its members against anti-selection. Emergency care – When should I call 911 or go to the emergency department? Call ER24 on 084124 if you are experiencing potentially life-threatening symptoms. These are some of the symptoms for which you should immediately call ER24;
What if I’m afraid to go to the emergency department? We understand those fears, but emergency department staff members wear personal protective equipment, and all places are fully cleaned and disinfected. Please note, that waiting too long to seek care for some health care emergencies is a bigger risk than the chance of contracting COVID-19. How do I know I won’t get COVID-19 in the emergency department? Depending on the urgency of the patient’s medical needs, everyone entering the emergency department is immediately screened for symptoms of COVID-19. How do I know I won’t contract COVID-19 if I need to stay in the hospital for treatment?
All labour and delivery patients – How are women protected whom come in for labour and delivery? In order to prevent the spread of COVID-19 and protect the health of all patients and staff members, testing for COVID-19 and taking precautions for each woman who is admitted to labour and delivery for delivery. The care team will follow special infection prevention procedures and wear proper personal protective equipment. Depending on the woman’s COVID-19 test results, she may be cared for in a special room and according to COVID-19 guidance for deliveries. What to expect when you go to the hospital During the COVID-19 pandemic, we have extra measures in place to prevent the spread.
Registration for COVID-19 Vaccine Acting health minister Mmamoloko Kubayi-Ngubane has announced a major boost to South Africa’s Covid-19 vaccination plans, with vaccines now being made available to more age groups and on weekends. Kubayi-Ngubane said that the government had also agreed to open vaccine registrations to people in the 35 – 49 age group.
All staff will be vaccinated, even if you’re not part of Discovery health, if they are part of company staff list, then they are eligible to receive vaccination. Should you be interested, please contact us and we will assist to communicate with Discovery to action Discovery Vaccination programme for employers.
Vaccination during riots and civil unrest period Please note that some of the vaccination sites that are affected are temporarily closed due to looting, riots and civil unrest. The vaccination rollout will be delayed but still encourage all clients to please use their digital form to register and make appointments. Those that missed their appointment due to recent looting will be rescheduled. If you have any other queries please contact our Health department, email service@daberistic.com, Tel 011-6581333, Option 2 for Medical Aid. |
AuthorKevin Yeh Archives
January 2025
Categories
All
|
-
I would like to
- Signup Newsletter
- Schedule an appointment
- Go to hospital
- Deal with an accident
- Make a Claim
- Invest >
- Apply for insurance >
- Appoint Daberistic as broker
- Promotions >
- Update my policy >
- Make a Will
- Set up a business
- Get an accountant.
- Get business tax advice
- Get personal tax advice
- Preferred Suppliers >
- Cancel Daberistic Services
- Covid-19 toolkit
-
Invest
- Our fund selection process
- Retirement annuity
- Tax-free Investment Plan >
- Unit Trusts
- Guaranteed Investments >
- Preservation funds
- Offshore
- Education plan
- Endowment
- Participation Bond
- Deposits
- Business investment accounts
- Private investment accounts
- Exchange Traded Funds
- Share investing
- Personalised share portfolio
- Retirement income
- Retirement Funds
-
Health
- Life
- Insure
-
Financial Coach
-
Accounting & Tax
-
About us
-
我想要
- 财富管理
- 员工福利
- 人寿保险
- 医疗保险
- 财产险
- 会计师事务所
- 关于我们
-
I would like to
- Signup Newsletter
- Schedule an appointment
- Go to hospital
- Deal with an accident
- Make a Claim
- Invest >
- Apply for insurance >
- Appoint Daberistic as broker
- Promotions >
- Update my policy >
- Make a Will
- Set up a business
- Get an accountant.
- Get business tax advice
- Get personal tax advice
- Preferred Suppliers >
- Cancel Daberistic Services
- Covid-19 toolkit
-
Invest
- Our fund selection process
- Retirement annuity
- Tax-free Investment Plan >
- Unit Trusts
- Guaranteed Investments >
- Preservation funds
- Offshore
- Education plan
- Endowment
- Participation Bond
- Deposits
- Business investment accounts
- Private investment accounts
- Exchange Traded Funds
- Share investing
- Personalised share portfolio
- Retirement income
- Retirement Funds
-
Health
- Life
- Insure
-
Financial Coach
-
Accounting & Tax
-
About us
-
我想要
- 财富管理
- 员工福利
- 人寿保险
- 医疗保险
- 财产险
- 会计师事务所
- 关于我们
Services |
About us |
Support
|




 RSS Feed
RSS Feed